A review of the development of In-Hospital Neutron Irradiator-1 and boron neutron capture therapy clinical research on malignant melanoma
Introduction
Boron neutron capture therapy (BNCT) is a binary targeting radiation therapeutic modality based on the nuclear capture and fission reactions that occur when the stable isotope boron-10 is irradiated with neutrons to produce high-energy alpha particles and recoiling lithium-7 nuclei (1). The basic principle of BNCT was initially put forward by the American biophysicist G. L. Locher in 1936. Boron agent and neutron source are two basic conditions of BNCT research and always been optimized during the past 82 years. For the boron agent part, two boron agents, sodium mercaptoundecahydrododecaborate (Na210B12H11SH; Na210BSH) (2) and L-p-boronophenylalanine (L-10BPA) (3), have been clinically utilized for the treatment of malignant brain tumors (4), malignant melanoma (5), head and neck cancer, lung cancer, hepatoma, chest wall cancer, and mesothelioma (6-8). Next generation boron agents have taken two directions: small boron molecules and boron-conjugated biological complexes (9). For the neutron source part, there was no specially designed reactor-based neutron source could be used for BNCT researches before IHNI-1. Even neutron beam facilities for BNCT had not generally been part of the original design specifications for research or test reactors (9), except Massachusetts Institute of Technology Research Reactor (MITR) and Brookhaven Medical Research Reactor (BMRR) (10). From 1990, a significant number of reactors were modified to incorporate epithermal neutron beam, by using the reactor core directly as the source for the epithermal neutron beam (11-20). The reactors power is from 100 to 45 MW.
However, scientists had gradually realized that the research reactor really could not be regarded as a friendly environment for complicated medical treatment (21). For doctors and patients, the large and medium sized research reactors are always located at the place far from the populated areas, so doctors and patients need a long journey for the treatment and high level of security might increase mental burden for the patients. On the other hand, clinical irradiation might share use of the neutron source with comprehensive nuclear technology applications according to the reactor operation schedule. For owner of the facility, construction and maintain of research reactors would very expensive and complex and specially trained engineers and researchers are needed to guarantee the safety and normal operation of the facility. So, the requirement of newly designed neutron source, which could be site in hospital, designated for BNCT clinical trials is urgent. Different approaches have been studied, including 252Cf spontaneous fission radioisotope source, accelerator-based neutron source, small sized reactor specially designed for BNCT, and etc.
China has a strong background of the development of miniature neutron source reactor (MNSR) (22). International Atomic Energy Agency (IAEA) gave suggestions for an BNCT reactor in the hospital in “Current Status of NCT” as early as in 2001 (23) as following: “Designing an extremely safe NCTR is possible by using already proven technologies. An optimized low power reactor could be an effective tool to be used in a medical center.” and “The reactor itself is safe in any anticipated accident conditions because of low power, limited operation time, low excess reactivity and inherent safety feature of large prompt negative temperature coefficient. Its operation and management cost would be lower than that for the equivalent medical accelerator”. In 1980s, China’s prototype MNSR (24) with features of intrinsic safety, low power, small sized, low investment and unattended operation was successfully developed and installed for the purpose of neutron activation analysis (NAA). After modification and optimization, such type of low power reactor can serve as the proper BNCT neutron source facilities, which could almost follow all the suggestions of BNCT reactor in the hospital given by IAEA.
Development of IHNI-1
IHNI-1 is a specially designed reactor-based neutron source for BNCT, based on the MNSR technique. The overall framework of IHNI-1 was designed by Prof. Yongmao Zhou. IHNI-1 was constructed by Beijing Capture Technology Co. Ltd (BCTC) with the support and guidance of China National Nuclear Corporation (CNNC) plus the active and devoted involvement of China Zhongyuan Engineering Corporation (CZEC), China Institute of Atomic Energy (CIAE), Northwest Institute of Nuclear Technology (NINT), and etc. (22). IHNI-1 got fuel loading permit and construction permit from National Nuclear Safety Administration (NNSA) in July 2008. The construction of IHNI-1 was completed and realized its criticality by the end of 2009 and IHNI-1 achieved full power in Jan 2010.
Site and scope (22,25)
The site of IHNI-1 is in the vicinity of CIAE, Fangshan District, Beijing, China. It is 2 km away from the supporting hospital and about 40 km away from downtown. The main building has a floor space of 477 m2, including neutron source facility, neutron beam facility, medical facility, relevant process rooms and labs, medical preparation room, offices, etc. The reactor facility part is 4 m (depth) ×10 m (width) ×18 m (length) with a building area of 175 m2 with one floor underground and two floors on the ground. The total building area of the facility is around 500 m2.
Major technical parameters
IHINI-1 is pool-tank type reactor based on modified MNSR with thermal power 30 kW (26,27). IHNI-1 has low enriched uranium deeply-undermoderated reactor core designed with full natural circulation cooling. Light water is used for cooling and moderating. Table 1 shows the main parameters of IHNI-1 (22,25).
Table 1
| Item | Value |
|---|---|
| Reactivity of center control rod (mk) | −6.40 |
| Reactivity of auxiliary control rod (mk) | −3.78 |
| Total reactivity worth of upper reflector (mk) | ~17.6 |
| Cold excess reactivity (mk) | 4.20 |
| Fuel temperature reactivity coefficient (°C) | −1.289×10−5 Äk/k (20~100 °C) |
| Coolant temperature reactivity coefficient (°C) | −9.532×10−5 Äk/k (20~30 °C) |
| Effective delayed neutron fraction | 8.32×10−3 |
| Prompt neutron removal lifetime (s−1) | 7.935×10−5 |
IHNI-1 has three horizontal neutron beams, one thermal neutron beam and one epithermal neutron beam for BNCT treatment, one beam for prompt-γ analyzation. IHNI-1 also has two vertical neutron beam facilities at reactor vessel (22,28). It takes only 2–3 min for the reactor power rising from 0 to 30 kW. Only one trained operator is needed for routine operation and no nuclear waste would be released to the environment. If IHNI-1 running at 30 kW, 2.5 hours a day and 4 days a week, one cage of fuel could be used more than 20 years (28). Figure 1 shows the structure of INHI-1.
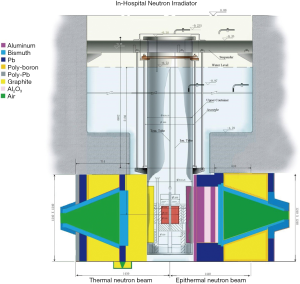
Composition of IHNI-1
IHNI-1 is composed of three modules, including miniature nuclear reactor neutron resource facility, neutron beam facility and support setups (22). The three modules will be introduced in detail as following:
Miniature nuclear reactor neutron resource facility
Reactor core (22 ,27 )
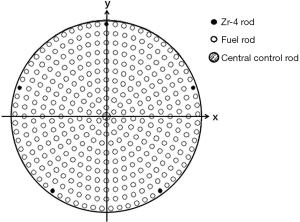
The reactor core is of 240 mm in height and diameter, respectively, and the core volume is 10.9 L only. The fuel cage of reactor core has 350 lattice positions in array of concentric circles and equi-radian length (Figure 2) and 302 integrated element rods are loaded. Element rods are made of highly sintered density UO2 pellets with 235U enrichment of 12.5%.
The reflectors are made of metal beryllium (27). The side reflector is one beryllium annulus installed vertically around the reactor core. The bottom reflector is one beryllium disc beneath the reactor core. The top reflector is made of beryllium sheets on the top of reactor core.
Control rod (22 ,28 )
One center control rod, one auxiliary control rod and two reactivity regulators are sited in the reactor. All of them are made of cadmium tube with aluminum layer inside with different size and design. The center control rod is installed at the center of the reactor core for the purposes of reactor startup, shutdown, reactor power adjustment as well as stable operation automatic control under rated power. The position of auxiliary control rod and reactivity regulators is inside the side reflector. The auxiliary control rod is designed for reactor shut down in case of center control rod failure or upper reflector operation. The reactivity regulators are set in the purpose of excess reactivity regulation and not involved in the operation control of the reactor.
Neutron energy regulator (22 ,25 )
Two arc-shaped neutron energy regulators, which are one graphite block and one aluminum block for thermal neutron and epithermal neutron beam, respectively, are arrayed in a radian range of 120° in the gaps between inside wall of the reactor vessel lower section and ex-annulus of the Be reflector. The mixed spectrum neutrons released from side reflector will be collected and intercepted by the regulator.
Reactor vessel (22 ,28 )
The cylinder-shaped reactor vessel is composed of upper and lower sections and locates at the center of the reactor water pool. Reactor core, beryllium reflectors, control rods, neutron energy regulators and reactor core parameters measurement device are installed in the lower section. The reactor vessel water surface is 5 meters above the top of reactor core. The volume of reactor water is 1,621.5 L. The nuclear fission heat produced by the core conducts to reactor water through natural convection, and then conducts through the vessel wall to the pool water.
Reactor water pool (22 ,28 )
The rectangular reactor water pool is set at the center of the reactor hall, with a volume of 40 m3. The water surfaces of the reactor pool and reactor vessel are to be maintained at the same level. The pool water is to let out heat produced from the reactor core and provides radiation protection to work staff.
Neutron beam facility
Three neutron horizontal beam facilities are designed in IHNI-1 (Figure 1). One thermal neutron beam and one epithermal neutron beam are branched out from left and right sides of side reflector around the core of IHNI-1, respectively. In the vertical direction of thermal neutron beam, tangential direction of the core, one measurement beam is branched out (22).
Thermal neutron beam facility
Thermal neutron beam energy field is <0.4 eV. The beam is composed of graphite filter, bismuth shield, boron poly, bismuth cone collimator and outside collimator (27). A conical cavity is designed to straighten neutron beam flow parallelly at beam port. Five adjustable apertures (6, 8, 10, 12 and 14 cm) are designed at the beam port. The primary γ-ray radiated from the core and the secondary γ-ray induced by components of beam will be absorbed by bismuth structure (22). Compared with metal lead, metal bismuth has the advantage of higher neutron availability and lower secondary γ-ray contamination compositions. A frustum-shaped outside collimator, 15 cm protruding from the wall level, is designed for eliminating thermal neutrons escaped to the outside and reducing normal issue dose of the patient. The set of outside collimator also makes positioning of the patient much easier than the beam port just on the wall. Thermal neutron beam facility can be used in in vitro and in vivo BNCT study as well as clinical trials of shallow tumor, such as cutaneous malignant melanoma.
Epithermal neutron beam facility
Epithermal neutron beam energy field is at the range from 0.4 eV to 10 keV. The beam is composed of aluminum filter, Al2O3 filter, cadmium absorbing curtain, bismuth shield, boron poly, bismuth cone collimator and outside collimator (25). The size and function of cone-shaped outside collimator is the same as thermal neutron beam, but the material is different according to different energy range requirements of the two beams. As thermal neutron beam, five adjustable apertures (6, 8, 10, 12 and 14 cm) are designed at the beam port. Epithermal neutron beam facility can be used for deeper tumor treatment, such as brain tumor, head and neck cancer, etc.
Thermal neutron measurement beam
Neutron beam energy field is <0.4 eV. The beam port is designed with a diameter of 2 cm. As the beam is at the tangential direction of the core, the primary γ-ray level is very low. Thus, the measurement beam is suitable for prompt γ-ray neutron activation analysis (PGRNAA) for real time boron concentration in the course of BNCT treatment.
Support setups
Irradiation room
Irradiation rooms of the size 2.0 m (H) × 4.0 m (W) × 4.6 m (L) have been designed for thermal neutron beam and epithermal neutron beam, respectively (22). The setups in the room are as follows:
- Operation bed for patient positioning at irradiation aperture from different directions;
- Neutron and γ-ray dose measuring and monitoring system;
- Monitor and intercom system for observing and communicate with the patient inside the irradiation room.
Position system
Position system is designed for exact localization and precise repetition of patient treatment position. Position system is composed of two parts, beam simulation facility and isocentre laser unit. The beam simulation facility is composed by a simulation collimator with the same size and height of outside collimator of the two beams and a beam-eye view window. The beam-eye view window is made of transparent polymethylmethacrylate (PMMA) and designed to help doctors to find and verify the irradiation field. Isocentre laser unit in simulation room is including one ceiling mounted and three side wall-mounted lasers. Isocentre laser unit in two treatment room is made up with one ceiling mounted and two side wall-mounted lasers for each room.
Boron concentration detection systems
Both PGNAA system and inductively coupled plasma-atomic emission spectrometer (ICP-AES) measurement system have been built in IHNI-1 for boron concentration detection. The PGNAA system is composed by an n-type HPGe detector of 40% efficiency, digital spectrometer and shielding part. For both detector shielding part and the neutron beam shielding part, the inner layer was Li2Co3 powder and the outer is lead (29). ICP-AES system is composed by iCAP 6300 ICP spectrometer and sample preparation devices. Boron concentration of blood sample, 4-dihydroxyborylphenylalanine-fructose (BPA-F) infusion sample, urine sample and tissue sample could be measure by two systems.
Irradiation detection systems
One p-type HPGe detector of 70% efficiency and 4πβ-γ system are site for neutron flux measurement. Thermo-luminescence detector (TLD) system is prepared for measurement and evaluation of γ-ray or the total dosage of gamma and neutrons.
Main test operation result of IHNI-1 (24,30)
After construction of all the IHNI-1 components including fuel, Be reflector, detectors, three neutron beams facilities, and etc., startup of IHNI-1 was realized in December 2009. The following is the main experimental results of the test operation of IHNI-1, which demonstrates that IHNI-1 has inherent safety and could provide long time stable neutron flux density for BNCT.
Power excursion experiment
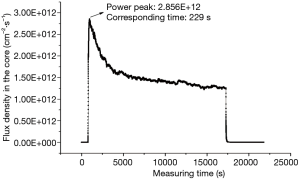
Safety of the IHNI-1 relies on a limited maximum excess reactivity control in normal and abnormal conditions. When a certain amount of positive reactivity is inserted into the reactor promptly, the power will be increased rapidly, however, it will turn to the normal value due to the negative temperature effect. Figure 3 shows the curve of power transient. The maximum peak power value for 4.2 mk reactivity release was 85 kW with the corresponding time 229 s, and then the power turned to normal level without any operation.
Long time operation at full power
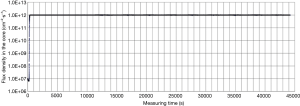
Figure 4 shows that at the full power of 30 kW, the IHNI-1 can be operated for 12 hours continuously, and the perturbation of the flux density was about 3‰, which demonstrated IHNI-1 could provide very stable neutron flux density for BNCT irradiation.
Characterization of IHNI-1 beams (31,32)
Basic characterization of the neutron beams of IHNI-1 was determined experimentally by research group from CIAE before clinical application, including neutron spectra, neutron fluence rate and its spatial distribution and the dosed induced by undesired neutrons and γ-rays of free neutron beams in-air.
Neutron spectra
An extended Bonner sphere spectrometer (BSS) was developed and the relevant experimental method was designed for the measurement of the neutron spectra of two treatment neutron beams with wide energy range, high flux density, strong room-scattering background and non-uniform neutron distribution. The BSS was based on a 3He proportional counter as thermal neutron sensor and consisted of 14 detection units. In order to improve the resolution in epithermal region, four polythene spheres covered with different thicknesses of boron shells were designed. The response functions of the spectrometer were calculated with the Monte Carlo N Particle Transport Code (MCNP), and calibrated and verified with standard 252Cf and 241Am-Be neutron sources. The measurements were performed at 110 cm from beam port. The neuron spectra at the beam port were deduced by anti-iteration technique.
Agreement between the measured and calculated spectra was fairly satisfied in the predominant energy ranges. The measured spectra showed a little increasing discrepancy with the calculated ones in the relative high energy ranges.
Neutron fluence rates
A system based on gold foils and an improved 235U fission chamber was established for measuring the neutron fluence rates of different energy regions. Thermal and epithermal neutron fluence rates were measured by gold foils, bare or cadmium-covered. Activities of the gold foils were determined by 4πβ-γ coincidence device. Fast neutron fluence rate was detected by Boron-covered 235U fission chamber. Results showed a good agreement of design. Thermal neutron fluence rate of thermal neutron beam was 1.90×109 cm−1·s−1and calculated values was 1.87×109 cm−1·s−1. Epithermal neutron fluence rate of epithermal neutron beam was 4.90×108 cm−1·s−1and calculated values was 5.03×108 cm−1·s−1.
Neutron spatial distributions
Neutron spatial distributions were measured by scanning manner with a bare 235U fission chamber for the thermal beam, for the epithermal beam with a cadmium-covered 235U fission chamber. The measurement results agreed with the simulated results. Neutron fluence rate was almost flat within the beam aperture (12 cm diameter). There was a central region with the diameter of 4 cm where the neutron fluence rate was within 95% of its maximum value.
Gamma kerma rates
A system based on TLD-600 (6LiF:Mg,Ti) and TLD-700 (7LiF:Mg,Ti) thermoluminescence dosimeters was established for measuring the air kerma rate of γ rays in the neutron beams with high flux density. The air kerma rate of undesired neutrons in the neutron beams was determined by means of the measured neutron spectra and neutron fluence rates together with the air kerma coefficients of neutrons. Measured values of gamma kerma rates were 1.01 Gy·h−1 and 1.05 Gy·h−1, respectively for thermal beam and epithermal beam. Measured values were higher than the calculated results.
Clinical research for malignant melanoma (33)
A clinical research for treating malignant melanoma by BNCT was designed by using IHNI-1 as the neutron source. This clinical research was approved by the Medical Ethics Committee of the Third Xiangya Hospital of Central South University and the research was conducted in accordance with the protocol as per ClinicalTrials.gov (No. NCT02759536)
The first patient was enrolled in August 2014. The patient got pigmented lesions on the sole and heel of his left foot and was diagnosed as malignant melanoma. He refused first-line treatment option and demanded to be enrolled as the first BNCT patient in China. The patient accepted an uptake study four days before BNCT irradiation, to get both tumor and normal tissue and blood samples to make sure the T/N, N/B, T/B factors. The patient’s organ at risk (OAR) was normal skin. The prescription dose of normal skin was 16 Gy-eq. BPA (produced by Syntagon AB) dose was 350 mg/kg with injection time 90 min. The dose calculation was carried out by using MCNP by modeling the targeting region of the patient and got a table of BPA concentration, OAR dose and treatment time. Some assumption was set in dose calculation as following: 10B concentration in blood (CB) would be measured before the treatment and get the result within 5 min; 10B concentrating in tumor (CT) was equal to T/B multiply by CB; 10B concentrating in normal skin (CS) was equal to N/B multiply by CB; 10B concentrating was homogeneous in both normal skin and blood; compound biological effectiveness (CBE) factors for normal skin and tumor were 2.5 and 3.8, respectively; relative biological effectiveness (RBE) factor for high linear energy transfer (LET) particle was 3.2.
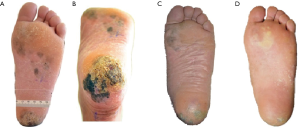
The patients were treated with two irradiation fields on his heel and sole of his left foot for one BPA-F infusion between 120–180 min after the beginning the infusion on September 9th 2014. The irradiation time was 10.5 and 12 min respectively for the two irradiation field. Only grade 2 acute radiation injury was observed during the first 4 weeks after BNCT and the injury healed after treatment. No late radiation injury was found during the 24-month follow-up. Figure 5 shows gross examination of the patient before and after BNCT. Based on positron emission tomography-computed tomography (PET/CT) scan, pathological analysis and gross examination, the patient showed a complete response to BNCT.
Conclusions
IHNI-1 is a specially designed reactor-based neutron source for BNCT, which could be set in hospital. IHNI-1 has the features of inherent safety, low power, small size, longtime stable, easy and quick operation and low investment for construction and maintain. The beam parameter measurement showed a good agreement of design value and could meet the requirement for BNCT irradiation. The first patient, treated by using IHNI-1 as the neutron beam source, showed a complete response to BNCT, preliminary indicating that IHNI-1 is a safe and efficient neutron source for BNCT.
BNCT is a novel method for cancer treatment. IHNI-1 makes it is possible for hospitals or medical research centers to equip with BNCT neutron source and carry out BNCT clinical research and we believe IHNI-1 would make its contribution to the development of BNCT research and application.
Acknowledgments
We thank Professor Yongmao Zhou for giving great effort in IHNI-1 development. We also thank Taiwan BNCT research group for giving long-term help and support for the BNCT development in the mainland of China.
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editors (Hiroaki Kumada and Yi-Wei Chen) for the series “Boron Neutron Capture Therapy” published in Therapeutic Radiology and Oncology. The article has undergone external peer review.
Conflicts of Interest: Both authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/tro.2018.10.03). The series “Boron Neutron Capture Therapy” was commissioned by the editorial office without any funding or sponsorship. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Barth RF, Vicente MG, Harling OK, et al. Current status of boron neutron capture therapy of high grade gliomas and recurrent head and neck cancer. Radiat Oncol 2012;7:146. [Crossref] [PubMed]
- Soloway AH, Hatanaka H, Davis MA. Penetration of brain and brain tumor. VII. Tumor-binding sulfhydryl boron compounds. J Med Chem 1967;10:714-7. [Crossref] [PubMed]
- Snyder HR, Reedy AJ, Lennarz WJ. Synthesis of Aromatic Boronic Acids. Aldehydo Boronic Acids and a Boronic Acid Analog of Tyrosine. J Am Chem Soc 1958;80:835-8. [Crossref]
- Nakagawa Y, Hatanaka H. Boron neutron capture therapy. Clinical brain tumor studies. J Neurooncol 1997;33:105-15. [Crossref] [PubMed]
- Mishima Y, Ichihashi M, Hatta S, et al. New thermal neutron capture therapy for malignant melanoma: melanogenesis-seeking 10B molecule-melanoma cell interaction from in vitro to first clinical trial. Pigment Cell Res 1989;2:226-34. [Crossref] [PubMed]
- Kato I, Ono K, Sakurai Y, et al. Effectiveness of BNCT for recurrent head and neck malignancies. Appl Radiat Isot 2004;61:1069-73. [Crossref] [PubMed]
- Aihara T, Hiratsuka J, Morita N, et al. First clinical case of boron neutron capture therapy for head and neck malignancies using 18F-BPA PET. Head Neck 2006;28:850-5. [Crossref] [PubMed]
- Suzuki M, Sakurai Y, Hagiwara S, et al. First attempt of boron neutron capture therapy (BNCT) for hepatocellular carcinoma. Jpn J Clin Oncol 2007;37:376-81. [Crossref] [PubMed]
- Harling OK, Riley KJ. Fission Reactor-Based Irradiation Facilities for Neutron Capture Therapy. In: Sauerwein W, Wittig A, Moss R, et al. editors. Neutron Capture Therapy. Springer, Berlin, Heidelberg, 2012:19-39.
- Godel JB. Description of Facilities and Mechanical Components: Medical Research Reactor (MRR). Brookhaven National Laboratory Report BNL 600 (T-173). Tech Rep Brookhaven Natl Lab 1960;1-64. [PubMed]
- Auterinen I, Hiismäki P, Kotiluoto P, et al. Metamorphosis of a 35-year-old TRIGA reactor into a modern BNCT facility. In: Hawthorne MF, Shelly K, Wiersema RJ. editors. Frontiers in neutron capture therapy. vol I. New York: Kluwer Academic/Plenum Publishers, 2001:267-75
- Blaumann HR, Calzetta-Larrieu O, Longhino JM, et al. NCT facility development and beam characterization at the RA-6 reactor. In: Hawthorne MF, Shelly K, Wiersema RJ. editors. Frontiers in neutron capture therapy. 1st edition. New York: Kluwer Academic/Plenum Publishers, 2001:313-7.
- Burn KW, Casalini L, Martini S, et al. An epithermal facility for treating brain gliomas at the TAPIRO reactor. Appl Radiat Isot 2004;61:987-91. [Crossref] [PubMed]
- Capala J, Stenstam BH, Sköld K, et al. Boron neutron capture therapy for glioblastoma multiforme: clinical studies in Sweden. J Neurooncol 2003;62:135-44. [Crossref] [PubMed]
- Liu HB, Greenberg DD, Capala J, et al. An improved neutron collimator for brain tumor irradiations in clinical boron neutron capture therapy. Med Phys 1996;23:2051-60. [Crossref] [PubMed]
- Liu YWH, Huang TT, Jiang SH, et al. Renovation of epithermal neutron beam for BNCT at THOR. Appl Radiat Isot 2004;61:1039-43. [Crossref] [PubMed]
- Nigg DW, Venhuizen JR, Wemple CA, et al. Flux and instrumentation upgrade for the epithermal neutron beam facility at Washington State University. Appl Radiat Isot 2004;61:993-6. [Crossref] [PubMed]
- Raaijmakers CP, Konijnenberg MW, Mijnheer BJ. Clinical dosimetry of an epithermal neutron beam for neutron capture therapy: dose distributions under reference conditions. Int J Radiat Oncol Biol Phys 1997;37:941-51. [Crossref] [PubMed]
- Rogus RD, Harling OK, Yanch JC. Mixed field dosimetry of epithermal neutron beams for boron neutron capture therapy at the MITR-II research reactor. Med Phys 1994;21:1611-25. [Crossref] [PubMed]
- Sakurai Y, Kobayashi T. The medical-irradiation characteristics for neutron capture therapy at the heavy water neutron irradiation facility of Kyoto University Research Reactor. Med Phys 2002;29:2328-37. [Crossref] [PubMed]
- Barth RF, Joensuu H. Boron neutron capture therapy for the treatment of glioblastomas and extracranial tumours: as effective, more effective or less effective than photon irradiation?. Radiother Oncol 2007;82:119-22. [Crossref] [PubMed]
- Zhou Y. Neutron Capture Therapy (NCT) and In-Hospital Neutron Irradiator (IHNI)-a new technology on binary targeting radiation therapy of cancer. Engineering Science 2009;7:2-21.
- IAEA-TECDOC-1223. Current status of neutron capture therapy. 2001:9-12. Available online: https://www-pub.iaea.org/MTCD/publications/PDF/te_1223_prn.pdf
- Zhou Y. The Miniature Neutron Source Reactor. IAEA-TECDOC-384. Vienna, 1986:89-98.
- Li Y, Xia P, Peng D, et al. Construction of In-Hospital Neutron Irradiator. Engineering Science 2012;8:17-9.
- Li Y, Xia P, Wang X, et al. Start-Up of the First In-Hospital Neutron Irradiator (IHNI-1) & Presentation of the BNCT Development Status in China. Proceeding of ICNCT-14. BuenosAires, Argentina: Comisión Nacional de Energía Atómica, 2010:371-4.
- Ke G, Sun Z, Shen F, et al. The study of physics and thermal characteristics for in-hospital neutron irradiator (IHNI). Appl Radiat Isot 2009;67:S234-7. [Crossref] [PubMed]
- Li Y, Xia P, Peng D, et al. Performance and characteristic of In-Hospital Neutron Irradiator. Engineering Science 2012;8:20-2.
- Zhang Z, Chong Y, Chen X, et al. PGNAA system preliminary design and measurement of In-Hospital Neutron Irradiator for Boron Concentration Measurement. Appl Radiat Isot 2015;106:161-5. [Crossref] [PubMed]
- Li Y, Peng D, Zou S, et al. Test operation of In-Hospital Neutron Irradiator. Engineering Science 2012;8:23-7.
- Chen J, Li C, Li W, et al. Neutron Spectra Measurement of IHNI-I BNCT Beam with Multi-sphere Spectrometer. Atomic Energy Science and Technology 2014;48:2127-32.
- Chen J, Li C, Song M, et al. Preliminary characterization of radiation fields of IHNI-1 for BNCT. Engineering Science 2012;8:106-12.
- Yong Z, Song Z, Zhou Y, et al. Boron neutron capture therapy for malignant melanoma: first clinical case report in China. Chin J Cancer Res 2016;28:634-40. [Crossref] [PubMed]
Cite this article as: Zhang Z, Liu T. A review of the development of In-Hospital Neutron Irradiator-1 and boron neutron capture therapy clinical research on malignant melanoma. Ther Radiol Oncol 2018;2:49.